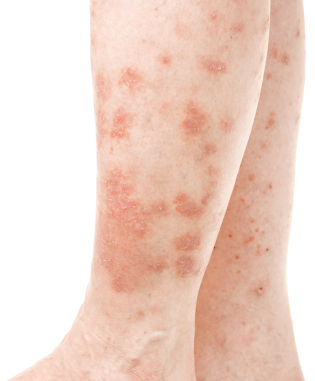
Living with eczema can be a battle on several fronts
You will not die from eczema. It is not a condition which typically has many research dollars put in its direction because people who do not have severe eczema do not comprehend that it really is impactful to your physical, mental, and emotional well-being, and that living with endless suffering — as in any condition — is not really an adequate quality of life. The sleepless nights with scratching, waking up with bloody sheets, showers that are painful and sore, itching with stress and sometimes itching for no reason at all, and not knowing the causes from one day and the next. The peeling skin from cortisone, and sometimes the need for cortisone shots, antihistamines, immunosuppressives to stop the immune response… these are all eczema realities. Being told you are doing something to elicit this, that you don’t want to stop, that you won’t feel better and that it somehow is related to self-control. Tell that to individuals with eczema. All they want is to stop scratching.
What your dermatologist won't tell you
Dermatologists do have an excellent knowledge of the skin because of course, as specialists, they are trained in that organ. However, sometimes when we look exclusively at an organ we are more apt to see symptoms only rather than cause. Eczema is a tough condition to crack, because where the pathology lies is often deeper than the skin’s surface. There absolutely are ways to reduce inflammation associated with eczema, and there are known triggers which can aggrevate an immune response. So why don’t you know about them?
- Not everyone with eczema is afflicted with the same triggers — This is unfortunately true. There are however a series of patterns which DO ring true, which I will discuss in a minute.
- Some of the things which can help eczema overall take time and patience. Many patients who are itchy and sore just want relief (I should know, I was one of them). Eventually however, you have to ask yourself, do you just want symptomatic relief or can you get to the bottom of the triggers?
- Triggers like food allergies that often go undiagnosed for those with eczema because the methods of testing are unfortunately not covered, or very rarely discussed within our medical system. OHIP does not cover either IgE blood testing for foods or IgG delayed-type hypersensitivity blood testing for foods, and as a result, it is expensive for patients to pay out-of-pocket for every potential trigger – and there can be many. IgE skin scratch tests offer mostly false negatives for those with skin issues – the skin is such a mess to begin with – it does not react when it is supposed to, and does when it should not.
So what are the triggers for eczema?
The breakdown in eczema is in the innate immune system. This is the part of the immune system that is responsible for telling the body what is foreign and what is not in the skin, lungs, and gastrointestinal tract from the moment we emerge from our mother’s womb. If you think about it, it makes sense as, when we are babies, these are the major ways we can succumb to infection. Unfortunately, if one part of this system is affected by something seen as “foreign”, then we know the other parts of the system are struggling.
In eczema, research demonstrates that the gastrointestinal tract is where this breakdown occurs, and can often occur before birth. Mothers given good bacteria or probiotics, and specific strains of probiotics that balance a very reactive innate immune system, do prevent and reduce the incidence of eczema in children of mothers with eczema or a genetic connection to eczema. Bacterial balance in the gastrointestinal tract is a very important part of eczema management.
Eczema breakouts do occur reliably with certain foods. These food groupings have allergy potential, and certain types of eczema are more prone to allergy (IgE-associated atopic dermatitis) versus those that are not IgE-associated (IgE is an immunoglobulin or protein produced by our body in the response to allergy). Dairy proteins, wheat and wheat gluten, tomatoes, citrus and citrus juices, nuts, certain fruits (apples from specific trees that have links to oral allergies, peaches and cherries from the prunus family) potatoes, and refined and synthetic sugars have all been linked to eczema. However, as there is such a range of individuals who react differently, evidence is mostly inconclusive. That does not however mean we should discount all of the research completely! It does mean that it will take more work to determine what is the cause. Food allergies are the leading culprit in eczema.
Hormone systems can also add to the mix, as stress and stress hormones have the ability to increase inflammation. Stress hormones and the hormone connection can also be an important contributor in eczema.
Chronic inflammation is an ongoing issue in eczema. Corticosteroids do help with local inflammation, but they do not support systemic inflammation. Important things like a good quality omega-3 oil can really support inflammation pathways and act like cortisone and cortisol, but also help to support the production of a good skin barrier. The skin barrier and its inability to stay intact and produce adequate oils as a protectant is an issue in eczema.
My immunosuppressives are doing the job, so why should I care about getting to the root cause?
Like anything, we have to wonder about too much of a good thing. Immunosuppressives like tacrolimus as in Protopic and Elidel are wonderful to get flare-ups under control, and at many points restore quality of life. The side-effects can be intense, and these interventions do have links to carcinogenesis. Yes, cancer. I am not trying to scare or prevent people from using these interventions when they need them as they do have positive safety profiles, and I myself used them quite a bit when I needed them. However, to prevent further risk from their use it is important to find the root cause.
What can you expect your life to look like with eczema when you find out your triggers?
You will have improved health, but patience is definitely a virtue. You may continue to need to rely on cortisone or other immunosuppressives but you may be able to reduce the amount that you depend on them. You may need to handle your stress differently than your friends. You may not be able to eat whatever you want, but let’s face it, who can? You will still need to apply good quality moisturizers (i.e. Pure + Simple, La Roche Posay, Eucerin, Cetaphil, Keri) to help with dryness and keep your skin barrier intact, but perhaps less as your skin barrier might be a little more resilient than it normally would be. You can expect to have an improved quality of life, which is ultimately what all of us endeavour to have. Keep strong, my friends! There is a light at the end of the tunnel.
References
- Baker BS. The role of microorganisms in atopic dermatitis. Clin Exp Immunol 2006; 144(1): 1-9.
- Benedetto A et al. Atopic dermatitis: A disease caused by innate immune defects. J Invest Derm 2009; 129: 14-30.
- Earls, A. Atopic dermatitis and its association with innate immunity. Integrative Health Practitioners 2010.
- Hultsch T, Kapp A, and Speigel J. Immunomodulation and Safety of Topical Calcineurin Inhibitors for the Treatment of Atopic Dermatitis. Dermatology 2005; 211: 174-187.
- Kremmyda LS et al. Atopy Risk in Infants and Children in Relation to Early Exposure to Fish, Oily Fish, or Long-chain Omega-3 fatty acids: A systematic review. Clinic Rev Allerg Immunol 2009.
- Saaf AM et al. Global Expression Profiling in Atopic Eczema Reveals Reciprocal Expression of Inflammatory and Lipid Genes. PLoS ONE 2008 3(12): e4017.